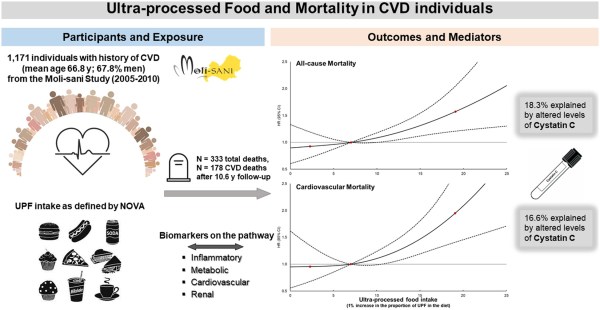
To evaluate the association of ultra-processed food (UPF) intake and mortality among individuals with history of cardiovascular disease (CVD) and analyse some biological pathways possibly relating UPF intake to death.
Methods and results
Longitudinal analysis on 1171 men and women (mean age: 67 ± 10 years) with history of CVD, recruited in the Moli-sani Study (2005–10, Italy) and followed for 10.6 years (median). Food intake was assessed using a food frequency questionnaire. UPF was defined using the NOVA classification according to degree of processing and categorized as quartiles of the ratio (%) between UPF (g/day) and total food consumed (g/day). The mediating effects of 18 inflammatory, metabolic, cardiovascular, and renal biomarkers were evaluated using a logistic regression model within a counterfactual framework. In multivariable-adjusted Cox analyses, higher intake of UPF (Q4, ≥11.3% of total food), as opposed to the lowest (Q1, UPF <4.7%), was associated with higher hazards of all-cause (hazard ratio [HR]: 1.38; 95% confidence interval (CI): 1.00–1.91) and CVD mortality (HR: 1.65; 95% CI: 1.07–2.55). A linear dose–response relationship of 1% increment in UPF intake with all-cause and CVD mortality was also observed. Altered levels of cystatin C explained 18.3% and 16.6% of the relation between UPF (1% increment in the diet) with all-cause and CVD mortality, respectively.
Conclusion
A diet rich in UPF is associated with increased hazards of all-cause and CVD mortality among individuals with prior cardiovascular events, possibly through an altered renal function. Elevated UPF intake represents a major public health concern in secondary CVD prevention.